The Office of Developmental Programs (ODP) is sharing this Health Alert to make all individuals, providers, staff, and other caregivers aware of the latest Health Alert from the Pennsylvania Department of Health (PA DOH) for Lyme disease and other tickborne illnesses.
The PA DOH notes that:
- Tick bite-related emergency department visits have increased recently in Pennsylvania.
- Health care providers should have a heightened clinical suspicion for tickborne diseases in persons with clinically compatible symptoms.
- Rare tickborne diseases, including hard tick relapsing fever and Powassan virus, continue to be found in ticks in multiple Pennsylvania counties, and human cases have been reported.
- Alpha gal allergy syndrome has been reported in Pennsylvania residents; health care providers should consider alpha gal allergy syndrome in persons presenting with mammalian meat allergies.
- For questions, please call 1-877-PA-HEALTH (1-877-724-3258) or your local health department for more information.
The PA DOH has identified recent sustained increases in tick bite-related emergency department visits in nearly all regions of the state. This trend was expected, as tick exposures in Pennsylvania generally increase during spring and summer months and serves as an important reminder that tickborne diseases occur seasonally in Pennsylvania. In addition, an increase in persons seeking care for Lyme disease (LD) is anticipated in the coming weeks to months as the peak period for LD is late May through early August.
What Is a Tick?
Ticks are small, hard-bodied parasitic arachnids that range in color from brown to black. They have four pairs of legs and a small head with a mouthpart designed to pierce the skin of their host. They can range in size from as small as a pinhead to as large as a dime after feeding and becoming fully engorged with blood. Most ticks go through four life stages: egg, six-legged larva, eight-legged nymph, and adult. After hatching from the eggs, ticks must eat blood at every stage to survive.

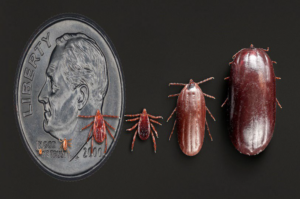
To attach to a host for feeding, they use their mouthpart to pierce the skin. The mouth part has small barbs that anchor it to the host.


What is a Tickborne Illness?
When a tick attaches to a person to feed, they can sometimes pass diseases that they acquired from another host. This is called a tickborne illness. Tickborne illnesses are caused by bacteria, viruses or other parasites passed to the host while the tick is feeding.
Symptoms of Tickborne Illness
Many tickborne diseases can have similar signs and symptoms. If you get a tick bite and develop the symptoms below within a few weeks, see your healthcare provider.
The most common symptoms of tick-related illnesses include:
- Fever/chills. All tickborne diseases can cause fever.
- Aches and pains. Tickborne diseases can cause headache, fatigue, and muscle aches. Peoplewith Lyme disease may also have joint pain.
- Rash. Lyme disease, Hard Tick Relapsing Fever, Powassan Virus, About Rocky MountainSpotted Fever | Rocky Mountain Spotted Fever (RMSF) , ehrlichiosis, Alpha Gal Syndrome,and tularemia can cause distinctive rashes.
Alpha-gal syndrome (AGS) is a serious allergy that can develop after a tick bite. It’s caused by your immune system reacting to a sugar molecule called alpha-gal (galactose-α-1,3-galactose), which is found in the bodies of most mammals — like cows, pigs, sheep, deer, and rabbits — but not in people.
How it Happens
When a tick bites, it can transfer alpha-gal from its saliva into your bloodstream. Your immune system may then recognize alpha-gal as a threat and start making antibodies to it. This sensitization can last for years.
When Symptoms Occur
- Food reactions: Often 2–6 hours after eating mammalian meat or products made frommammals (e.g., beef, pork, lamb, venison, rabbit, gelatin, some dairy).
- Non-food reactions: Some people react immediately to intravenous drugs, vaccines, orother products containing alpha-gal.
- Not everyone who gets bitten by a tick will develop AGS — the reason is not fully understood.
Tick Bite Prevention and Removal
Individuals with exposure to wooded and brushy areas with high grass and leaf litter are at greatest risk of tick exposure. The risk of getting a tick bite can be reduced by:
- walking in the center of trails and avoiding areas with high grass and leaf litter
- using EPA approved insect repellents on exposed skin and over clothing
- using products that contain 0.5% permethrin on shoes, clothing, and gear
- wearing light-colored clothing, which will make it easier to see crawling ticks
- conducting full-body tick checks (including pets) after spending time in tick habitats
- bathing or showering within 2 hours after coming indoors; and
- placing clothing worn outdoors in the dryer on high heat for 10 minutes to kill ticks.
If an attached tick is found, it should promptly be removed using fine-tipped tweezers. The tick should be grasped as close to the skin’s surface as possible and pulled upward with steady, even pressure. CDC’s directions for tick removal can be found at What to do after a tick bite.
It is common for individuals who remove a tick to want it to be tested. However, testing of individual ticks is discouraged for the following reasons:
- If the tick tests positive for disease-causing organisms, that does not necessarily mean that the bitten individual has been infected.
- If the bitten individual has been infected, they are likely to develop symptoms before results of the tick test are available. Patients with symptoms should not wait for tick testing results before starting treatment. Negative results can lead to false assurance. For example, the individual may have been unknowingly bitten by a different tick that was infected.
- After sharing these limitations, if a person still would like to have the tick tested, they can find more information on tick testing here: Avoid: Testing of ticks.
Contact your healthcare professional if:
- You can’t completely remove the tick. The longer the tick remains attached to the skin, the greater the risk of getting a disease from it. Your skin may also get irritated.
- The rash gets bigger. A small bump may appear at the site of the tick bite. This is typical. If it develops into a larger rash or you develop a rash anywhere, possibly with a bull’s-eye pattern, it may be a sign of Lyme disease. The rash usually appears within 3 to 14 days.
- Consult your provider even if the rash disappears because you may still be at risk of having the disease. Your risk of contracting a disease from a tick bite depends on where you live or travel to, how much time you spend outside in woody and grassy areas, and how well you protect yourself.
- You develop flu-like signs and symptoms. Fever, chills, fatigue, muscle and joint pain, and a headache may accompany the rash.
- You think the bite site is infected. Signs and symptoms include pain, change in skin color or oozing from the site.
- You think you were bitten by a deer tick. You may need antibiotics. If possible, bring the tick, or a photo of the tick, with you to your doctor’s appointment.
References
Lyme Disease and Other Tickborne Diseases in Pennsylvania
Ticks | Ticks | CDC
Tick bites: First aid – Mayo Clinic



